Uterine Rejuvenation with PRP
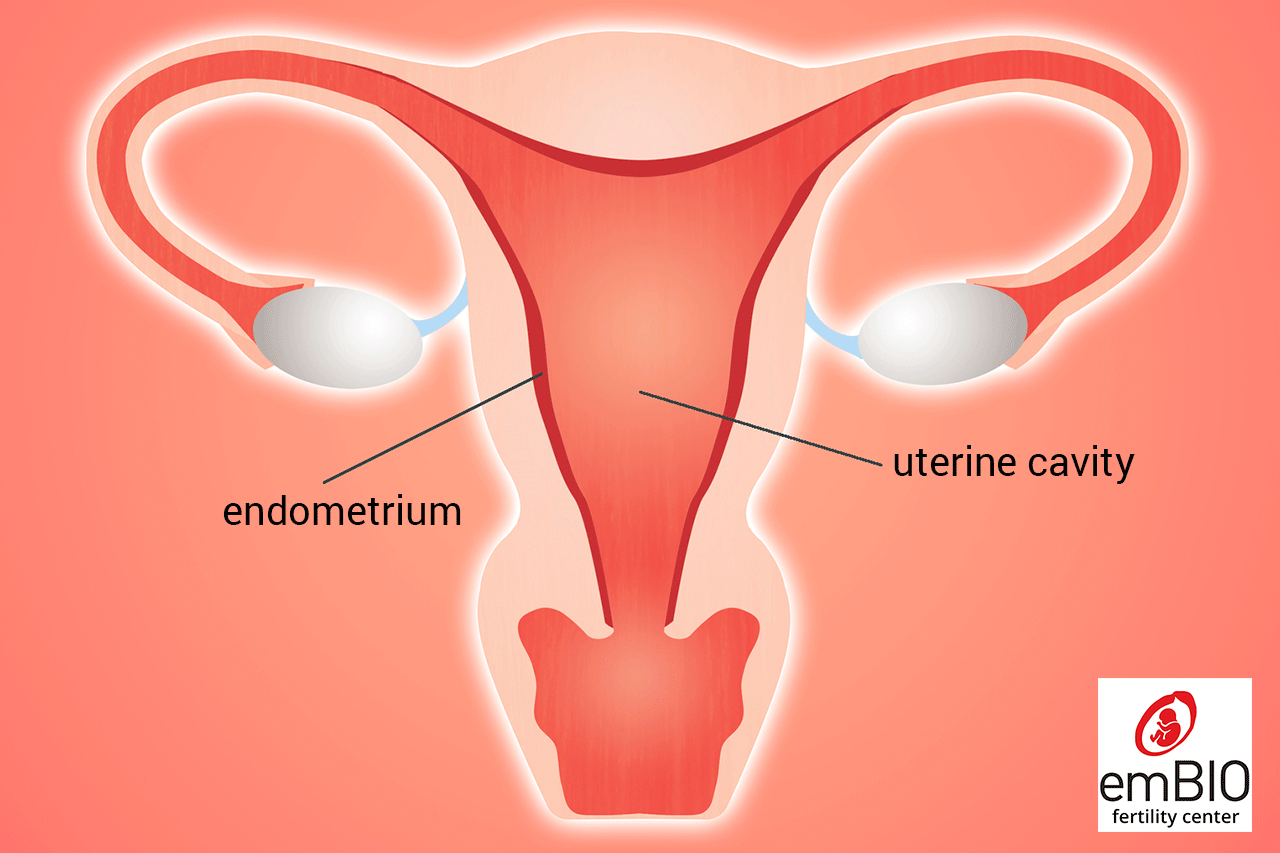
Uterine Rejuvenation with PRP is a medical treatment known also as endometrial rejuvenation or endometrial regenerative therapy, which aims to improve the thickness and health of the uterus lining (endometrium).
Adequate thickness of the uterine lining is crucial for pregnancy, and a thin lining can negatively affect the chances of embryo implantation after IVF. For individuals undergoing in-vitro fertilization (IVF), having an adequate endometrial thickness is particularly important.
In vitro fertilisation involves fertilising the egg outside the body and then transferring the resulting embryo back into the womb. Thin endometrium can make it difficult for the embryo to attach and grow, leading to failed implantation or early pregnancy loss.
Advantages of Uterine Rejuvenation with PRP
- innovative treatment
- affordable
- simple and easily performed
- effective
- non-invasive
- no side effects
As with all innovative treatments, more research is required to fully understand their potential and safety. However, several studies have shown that PRP can effectively improve pregnancy rates.
For instance, in a study by Chang et al., all 5 patients who underwent PRP therapy experienced effective endometrial thickening, and they all conceived.
According to another study by Nazari et al., -16 out of 20 women who underwent PRP therapy became pregnant.
In the field of reproductive health, Endometrial Regenerative Therapy is a beacon of innovation, offering a ray of hope to people facing various challenges on their journey to parenthood.
Through the remarkable regenerative potential of platelet-rich plasma, this therapy demonstrates the power of harnessing the body's own healing mechanisms to restore and rejuvenate uterine tissue, thereby increasing the chances of successful pregnancies.
Read how Penny became pregnant after endometrial rejuvenation with PRP
How does the endometrium affect implantation?
The endometrium plays a critical role during implantation, and there is a biochemical communication between the endometrium and the blastocyst at the time of the implantation process. Hormones such as estrogen and progesterone prepare the endometrium for implantation by thickening its lining.
Endometrial thickness is typically measured on ultrasound and is observed to increase as the cycle progresses. It is generally expected to reach a thickness of around 8-12 millimeters just before ovulation. This thickness allows for optimal conditions for embryo implantation.
A thin endometrial lining, typically defined as less than 7 millimeters, may indicate a lack of adequate blood flow and hormonal support necessary for successful implantation. In such cases, the chances of embryo implantation and subsequent pregnancy can be significantly reduced.
What are the common causes of thin endometrium?
There are many reasons why the endometrial lining may be less than optimal:
- Aging: As with many bodily functions, the reproductive system can show signs of wear and tear with age.
- Uterine scarring: Surgery or infection can sometimes cause scarring that affects the health of the endometrial lining.
- Long-term medications or treatments: Certain medicines or treatments, especially for cancer, can affect the uterus.
- Asherman's syndrome is characterised by the formation of intrauterine adhesions and it represents a significant obstacle to conception. Endometrial Regenerative Therapy represents a novel approach to the treatment of this syndrome. By harnessing the regenerative properties of PRP, the therapy aims to restore the endometrium, potentially reducing adhesion formation and increasing the chances of successful conception.
Which women are eligible for uterine rejuvenation?
You may be eligible for PRP therapy if you:
- are between the ages of 18 and 45
- have had a history of postponed embryo transfer due to insufficient thickness of the endometrium
- have had a history of two or more unsuccessful embryo transfers
- have a normal uterus with an endometrial lining of less than 7mm
- are planning to undergo IVF with embryo transfer
- your hemoglobin is higher than 11 g/dL and your platelets are more than 150,000/mm3
Not eligible for this treatment are:
- women diagnosed with cancer in the past
- women on any anticoagulation medicines or NSAIDs
Is uterine rejuvenation an easy process?
Endometrial Rejuvenation is a simple procedure and can be done 4-5 days before embryo transfer.
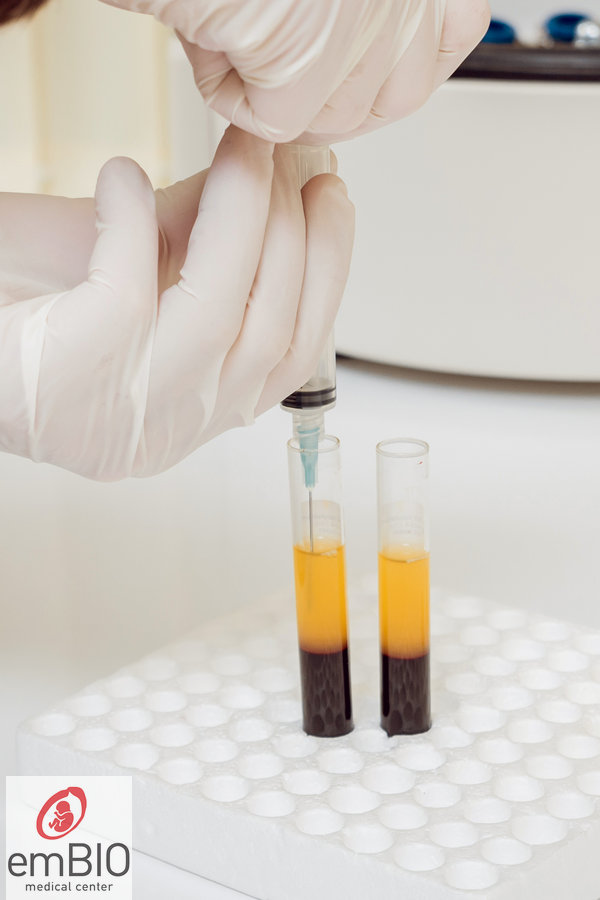
- After the necessary tests, 8-10 ml of blood is drawn from the vein
- The blood is then centrifuged twice, at 1500g for 10 minutes and then at 1000g for 10 minutes, to separate and prepare the Platelet Rich Plasma (PRP)
- This plasma enriched with platelets is infused into the uterine cavity via a catheter
- After a 15-minute rest, you are free to leave the clinic and return to your normal activities
- Endometrial thickness is re-assessed 48–72 hours later, and if it is not satisfactory, infusion with PRP can be performed another 1-2 times.
Free Online Consultation with Dr Thanos Paraschos and his team
Ultra-Enriched PRP Plasma
The EmBIO Fertility Center has improved the PRP procedure's efficacy through the research of its scientific expert team. To increase the effectiveness of PRP plasma, we isolated cytokines and growth factors from platelets. So far, our data show an increase of up to 1,000% in the beneficial effect of PRP on ovarian rejuvenation and endometrial thickening.
Schedule your appointment at EmBIO Fertility Center today and learn about the benefits of the new ultra-enriched PRP therapy in person!
Related Studies and Research
Lin et al. Platelet-Rich Plasma as a potential new strategy in the Endometrium Treatment in Assisted Reproductive Technology. Front. Endocrinol 2021;12:707584
Zamaniyan et al. Effect of platelet-rich plasma on pregnancy outcomes in infertile women with recurrent implantation failure: a randomized controlled trial. Gynecological Endocrinology 2021;37(2):1-5
Maleki-Hajiagha et al. Intrauterine infusion of autologous platelet-rich plasma in women undergoing assisted reproduction: A systemic review and meta-analysis. Journal of Reproductive Immunology 2020;137:1-9
Samy et al. Effect of autologous platelet-rich plasma transfusion for treatment of infertile women with thin endometrium and its implications in IVF cycles: a literature review. Middle East Fertility Society Journal 2020;25:5
Wang et al. Investigation of platelet‐rich plasma in increased proliferation and migration of endometrial mesenchymal stem cells and improving pregnancy outcome of patients with thin endometrium. J Cell Biochem 2019;120:7403-7411
Kim et al. Effect of Autologous Platelet-Rich Plasma Treatment on Refractory Thin Endometrium During the Frozen Embryo Transfer Cycle: A Pilot Study. Front Endocrinol 2019;10:61
Nazari et al. Effects of autologous platelet-rich plasma on implantation and pregnancy in repeated implantation failure: A pilot study. International Journal of Reproductive BioMedicine 2016;14(10): 625-628

