IVF Protocols for Ovarian Stimulation
During an IVF cycle, certain medications are used to stimulate the ovaries to produce many eggs. Doctors may give these medications in a variety of combinations called protocols.
In conventional IVF, two protocols are commonly used: the long and the short protocol. The drugs used in both protocols are the same; however, the dosages and the period of drug administration are different. The physician reviews the patient's records (woman's age, response to the medication and the outcome of previous attempts) and determines which protocol will be used for the upcoming treatment cycle.
Contents
Long Protocol
Ovarian Suppression
To optimize the stimulation of the ovaries, certain drugs (buserelin, leuprorelin, triptorelin, cetrorelix and ganirelix) are given starting approximately 1 week before the expected period, day 21 of a 28-day cycle. Alternately, patients can begin taking these drugs on day 2 of the cycle. These medications act by suppressing two hormones made in the pituitary gland, which normally cause your ovary to make eggs and ovulate. By suppressing these two hormones called Follicle Stimulating Hormone (FSH) and luteinizing hormone (LH), the ovaries become suppressed so that they do not make eggs nor produce the ovarian hormone called estradiol.
Women take these drugs for approximately 10-15 days. At the end of this period, an ultrasound scan of the uterus and the ovaries and a blood estradiol test are performed. If down-regulation is not complete, at approximately 10% to 15% of all cases, patients extend the same medications for another week. A second ultrasound scan and blood estradiol test are then performed. Occasionally, ovarian cyst aspiration is required.
Down regulation or ovarian suppression (the ovaries do not contain follicles greater than 15 mm in size, and the blood estradiol level is less than 50 pg/ml) allows the physician to have greater control over the ovarian stimulation. This provides for even growth of ovarian follicles and prevents a condition known as premature luteinization, defined as the premature attempt of the body to ovulate.
Free Online Consultation with Dr Thanos Paraschos and his team
Ovarian Stimulation
After ovarian suppression has been achieved, ovarian stimulation using synthetic follicle stimulating hormone fertility medication (Recombinant synthetic follicle stimulating hormone preparations, biguanide (oral type 2 diabetes medication), Menotrophin and follicle-stimulating hormone - FSH) may commence at a scheduled time referred to as the cycle start. On the cycle start day, your doctor may instruct you to reduce the initial dose, which will continue throughout the stimulation phase of the cycle until hCG is administered.
The dose of the medications is based on the woman's age, weight, the number of ovaries, FSH and estradiol levels and response to previous stimulation cycles. Patients take this initial dose of medication for 2 days before returning on the morning of synthetic follicle stimulating hormone Day 3 for an estradiol blood test. The dose may be changed then based upon the level of estradiol.
Women take medication for 2 more days before returning on medication on Day 5 for an estradiol blood test. Ultrasound scans are conducted starting on Day 7 of the stimulation period. In general, patients return for follow-up ultrasounds and estradiol blood tests, usually every 1 to 3 days, to monitor the growth of the follicles. Towards the end of ovarian stimulation, patients are asked to return to the clinic more frequently for observation. Most women require 8 to 12 days of ovarian stimulation plus 4 to 6 sonograms and/or estradiol levels. During ovarian stimulation, the drugs for down regulation (phase 1) are continued. Monitoring of ovarian stimulation (ultrasounds and blood tests) is conducted at our clinic.
Follicle Triggering (hCG)
When the growing follicles have met the criteria that indicate that the eggs are mature, patients are instructed to take hCG (human chorionic synthetic follicle stimulating hormone). Generally, at least two follicles with a mean diameter of at least 18 mm and an appropriate estradiol level (150-200pg/ml for each follicle) must be present before hCG is administered. Patients are instructed to inject hCG (5,000 - 10,000 units) approximately 36 hours before the oocyte retrieval. For example, if hCG, a human chorionic synthetic follicle-stimulating hormone, is injected at 7:00 p.m. Monday evening, oocyte retrieval will occur at 7:00 a.m. Wednesday morning. In addition, patients stop administering synthetic follicle-stimulating hormone and GnRH analogues after they have received hCG. Administration of hCG is commonly called follicle "triggering." This medicine aims to induce the final stages of oocyte maturation and the release of the eggs by the ovary. Timing of medication administration is important, and patients must follow the physician's and nurse's instructions carefully.
Short Protocol
The short protocol generally matches with the normal cycle and is, therefore, over a timescale of approximately 4 weeks (rather than the long protocol of 6 weeks). We prefer the short protocol when a woman has a poor ovarian response in previous cycles under the long protocol or where the woman is a bit older than average.
The main difference between the short and long protocols is that there are 2 distinct stages (down-regulating and stimulating) in the long protocol. In the short protocol, patients go straight to the stimulating stage. On day 3 of the cycle, patients usually go to the clinic for a scan and/or blood test to ensure that the womb lining has thinned out after their last period. Assuming that it has, they then start the stimulation injections described above and take the down-regulating nasal spray or injection simultaneously. Patients are then asked to return to the clinic after a few days and will have regular scans and blood tests (daily, every 2 days, or every 3 days) until the doctor decides they are ready for egg collection.
Once the fertility specialist has made that decision, the process is exactly the same as the long protocol described above (hCG injection, egg collection). The advantages of the short protocol are:
- fewer drugs to take as you skip the initial down-regulating stage
- a faster treatment cycle
Most women who have not had a good response under the long protocol find that they produce more eggs under the short protocol, but this is not always the case.
Follicle Stimulating Hormone (FSH) Injections
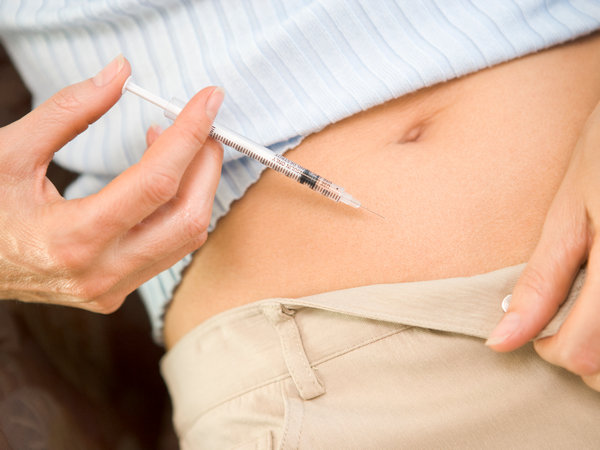
These injections are administered as a single subcutaneous injection in either the abdomen or thigh on an evening.
Biguanide oral type 2 diabetes medication
Comes in pen form. Either 300iu, 450iu&900iu. When using a new pen, remove the sheath from the needle and twist the needle onto the end of the pen. Dial to 37.5, pull out the end of the pen and press the end of the pen. This is to prime a new pen to ensure you then receive your full daily dose of biguanide (oral type 2 diabetes medication). Once the pen is primed, dial up your daily rose of biguanide, pull the end of the pen out, pierce the skin and press down the end of the pen to inject. Hold the needle in the skin for a couple of seconds before removing it. Remove the needle and place it in a sharps container for disposal. Only when opening a new pen do you need to prime it. A small amount of overfill may be left in the pen once the full amount is dispensed; you are not advised to administer this.
Recombinant synthetic follicle stimulating hormone preparations
Comes in pen form. Either 300iu, 600iu& 900iu. Remove the outer cover of the pen and cartridge from the packaging. Untwist the pen so the cartridge can be inserted and replaced. Remove the sheath from the needle and twist it onto the end of the pen. If you do not see a drop on the end of the pen, twist one click of the dosage dial and press the injection button. Dial up your daily dose of Recombinant synthetic follicle stimulating hormone preparations (FSH), pierce the skin and press down the end of the pen to inject. Hold the needle in the skin for a couple of seconds before removing it. Remove the needle and place it in a sharps container for disposal. A small amount of overfill may be left in the cartridge once the full amount is dispensed; you are not advised to administer this.
Uro Recombinant synthetic follicle stimulating hormone preparations - FSH and lutropin alfa - LH
- 75iu 1 powder to be mixed with 1ml of solvent (one ampoule)
- 150iu 2 powders to be mixed with 1ml of solvent (one ampoule)
- 225iu 3 powders to be mixed with 1ml of solvent (one ampoule)
- 300iu 4 powders to be mixed with 1.5ml of solvent (one and a half ampoules)
- 375iu 5 powders to be mixed with 1.5ml of solvent (one and a half ampoules)
- 450iu 6 powders to be mixed with 1.5ml of solvent (one and a half ampoules)
Please note: Some women will continue to experience bleeding whilst taking the FSH injections. Continue your injections, and please inform your ultrasonographer and nurse at your first appointment.
Free Online Consultation with Dr Thanos Paraschos and his team
Medications used in Infertility Treatment
Fertility doctors want to control the women's menstrual cycle to produce more mature oocytes. Several different drugs are used in the treatment cycles. Because each woman is unique, the drugs may vary even from cycle to cycle. The most common drugs used are:
A) GnRH analogues (agonists, antagonists)
These drugs down-regulate the pituitary gland and suppress the production of the hormones normally produced by the brain (LH and FSH), therefore controlling the stimulation of the ovary and preventing premature ovulation. Daily injections or nasal-inhalation of medications such as buserelin, leuprorelin, triptorelin, cetrorelix and ganirelix are usually started on the first day of the menstrual cycle and last for approximately 10 to 15 days. At the end of this period, down-regulation is complete. However, 20% of the women undergoing IVF treatment have to take the GnRH analogues longer to achieve down-regulation. This is mainly due to the presence of ovarian cysts that secret estrogens. These cysts are easily treated and do not affect the rest of the treatment.
B) Synthetic follicle stimulating hormones
The second phase of the IVF treatment is ovarian stimulation, which starts once down-regulation is confirmed. Various synthetic follicle-stimulating hormones like Menotrophin and follicle-stimulating hormone - FSH are prescribed daily to hyper-stimulate the ovaries to produce more mature oocytes. These drugs are usually injected, and their dose depends on the woman's age and her response to the medication.
C) Other Drugs
The last drug of an IVF treatment is Human Horionic Synthetic Follicle Stimulating Hormone (hCG), commonly known as hCG, human chorionic synthetic follicle stimulating hormone, which is injected at a specific time once the ultrasound scans show that at least three follicles have matured to 18mm in diameter. This drug triggers final follicular maturation and induces ovulation 32-36 hours later.
An antibiotic called doxycycline might be prescribed to the husband when ovarian stimulation begins and also to the wife after egg collection.
Finally, after embryo transfer, natural progesterone is exogenously provided in all IVF cycles to support the luteal phase, prepare the uterus for embryo implantation and stabilize the endometrium during pregnancy.
The New Follicle Stimulation Therapy with a Single Injection
The new follicle stimulation therapy with Recombinant Synthetic Follicle Stimulating Hormone Preparations makes things easier for women seeking to achieve pregnancy through an IVF protocol.
Instead of seven injections to stimulate the ovaries to produce enough mature eggs for a successful IVF treatment, now a single injection is enough.
What are Recombinant Synthetic Follicle Stimulating Hormone preparations?
It's a new type of recombinant follicle-stimulating hormone (rFSH), the hormone produced naturally in a woman's body, which stimulates the production of oocytes in the ovaries. The crucial difference is that in a natural menstrual cycle, only one mature egg is produced. In contrast, more eggs are opted for assisted reproduction technology (ART) to ensure maximum success rates. The major advantage of the new ovarian stimulation treatment is that 1 dose lasts for 7 days.
Is it as effective as the daily dose rFSH?
In the largest double-blind fertility agent trial in IVF run to date (Engage trial), it was shown that the rate of ongoing pregnancies achieved with the single-dose, 7-day lasting rFSH preparation, in combination with a GnRH antagonist protocol, was at least as effective (38.9%) as the daily dose preparation (38.1%). Other findings worth mentioning were a high number of eggs and good-quality embryos.
Advantages of the new rFSH
- Easier fertility therapy
- Although a COS therapy with Recombinant synthetic follicle stimulating hormone preparations must always be under the supervision of an infertility specialist, the patient may be trained to administer the injection herself or with the help of her husband.
- Minimized risk of error in dose
- Less stress is related to the time of the day the injection is administered. Combined with a GnRH antagonist protocol, Recombinant synthetic follicle stimulating hormone preparations may reduce the number of injections up to 70% within a fertility therapy cycle.
- One out of three patients may not require another Recombinant synthetic follicle stimulating hormone preparations injection after the initial one.
Frequent Questions regarding IVF Protocols
- Women with low AMH or high FSH
-
To maximize success rates with in vitro fertilization, we want a good number of high-quality eggs from the woman. We generally want about 8-15 eggs during the egg retrieval procedure.
IVF success rates correlate with the number of eggs retrieved with IVF.
Several ovarian stimulation medication protocols are used to "pump up" the ovaries to make sufficient follicles and eggs. Without stimulating medications, the ovaries will only produce one follicle and mature egg per menstrual cycle (month).
All of the commonly used IVF regimens include injections of a medication containing follicle stimulating hormone - FSH. Injectable FSH products are sometimes referred to as "synthetic follicle stimulating hormones", or Human Menopausal Synthetic Follicle Stimulating Hormones, HMG.
The woman is stimulated with the injectable FSH medications for about 8-12 days until multiple mature size follicles have developed.
- What is the goal of a good IVF ovarian stimulation?
-
With ovarian stimulation for in vitro fertilization, the goal is to produce approximately 8 to 15 follicles that will give quality eggs during the egg retrieval procedure.
We do not want to have overstimulation of the ovaries, which can lead to significant discomfort for the woman and, in rare cases, can result in ovarian hyperstimulation syndrome, OHSS.
We also do not want the ovarian stimulation to be insufficient and only give us a few eggs if we might have been able to obtain more by using higher medication doses, etc.
IVF can be successful with a very low number of eggs retrieved, but IVF Success rates are substantially higher when more than a few eggs are recovered.
With the ovarian stimulation, the task of the fertility specialist is to:
- Select a proper medication protocol and dosing regimen
- Monitor the patient's stimulation progress so that medication doses can be adjusted properly
- Trigger with hCG at the ideal time. Triggering too early or too late reduces success and can sometimes increase the risk for ovarian hyperstimulation (if triggered late). Most mature-sized follicles (about 15-20 mm in diameter) will give mature eggs at retrieval.
-
Quality control throughout the entire process is very important with in vitro fertilization. One of the ways that we have improved quality control in our program is by using highly specialized ultrasound equipment.
- How is the monitoring of the IVF stimulation done?
-
We try to stimulate the woman to get at least 4 follicles with sizes of 14-20mm in diameter. Ideally, there would be at least 8 follicles between 13-20 mm for IVF.
- The stimulating process usually takes about 8-10 days and our goal is to get a good number (about 8-15) of quality eggs.
- Blood hormone levels and developing follicle sizes are monitored. Ultrasound measures the follicles (discussed above on this page).
- Estrogen hormone blood levels are important. Estrogen (actually estradiol) levels are usually under 60 pg/ml at cycle baseline and rise significantly as multiple follicles develop.
- Peak estradiol levels in IVF at the time of HCG are usually between 1000 and 4000 pg/ml. Estradiol starts low and rises to 1000 to 4000 pg/ml by the time of the HCG injection.
- The HCG injection is given when the estrogen level and the follicle measurements look best for a successful IVF outcome. The HCG shot is needed to induce final egg maturation.
- The egg retrieval is planned for 34-35 hours after HCG injection - shortly before the woman's body might start to release the eggs (ovulate).
- How many follicles do you need to get pregnant with IVF?
-
Usually, it is not difficult to get enough follicles to develop. However, sometimes the ovaries' response is poor - and a low number of growing follicles are seen. The ovaries' ability to stimulate and make numerous follicles can be predicted fairly well by an ultrasound test - the antral follicle count.
The minimum number of follicles needed to proceed with IVF treatment depends on several factors, including follicle sizes, age of the woman, results of previous IVF stimulations and the willingness of the couple (and the doctor) to proceed with egg retrieval when there is a low number of eggs obtained.
In our experience, IVF success rates are very low with less than 3 mature follicles.
Some IVF doctors will say that you should have at least 5 follicles of 14mm or greater, while others might do the egg retrieval with only one follicle.
Women who are more likely to be low responders to ovarian stimulation would be those with low antral follicle counts, women who are older than about 37, women with elevated FSH levels, and women with other signs of reduced ovarian reserve.
Book a Free Online Consultation with Dr Thanos Paraschos and his team

